As with most adults during this quarantining/social-distancing era, mornings begin by reading some periodical(s) concerning the pandemic, and where we are supposed to go to work today… or, if there is a job to go to? Oh, and what about the kids, the therapies, the doctors and medications, and what to do about education? Updates from the New England Journal of Medicine and The Journal of the American Medical Association, are a new daily addition to my normal morning fare. So, with 5 decades of pediatric experience, including more than 10 years of treating developmentally-challenged youngsters, and listening to hundreds of families’ concerns and issues regarding the “Where should my child go next year?” question, I wanted to provide a framework for answering the riddle. In the absence of a great deal of certain science, this matrix should assist parents in making the best-informed decision for their child who requires special accommodations or other academic and social needs.
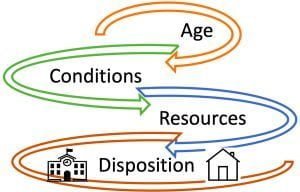
AGE
Toddlers 2-3 It’s probably best to remain home. There will be fewer cooties overall, and masks aren’t so helpful when babies are… being babies.
Young children 3-4 If the child is speaking but requires peer socialization, short periods of time going to a small preschool may be worthwhile. Depending on schedules, I have found few affected patients who can really Zoom for any useful period of time. For those with significant language delay, ABA and Speech Therapy must somehow be provided. Parents should worry less about academics at such a juncture.
Youngsters 4-6 As socialization becomes increasingly important, academic pursuits are often stressed at school. At home, the families’ abilities to fulfill that need (time, patience, other resources) must factor into the possible risks from returning to a schoolroom. At this juncture, language and behavioral delays should take precedence over a worry that, “the child won’t catch up” with scholarship.
Children 6-8 Anxiety can lead to learning problems for many socially inadequate/awkward patients. At this age, given the stresses that may come from returning to a strange classroom with unforeseen obstacles, another school year spent at home might be the correct decision. Parents may ask themselves, “Did the child learn better during Quarantine?” If so, resources become the most pressing factor in deciding Junior’s next step. As social, school, and other services open safely, that will offer some return to academic reality.
Children 8-12 As children move toward adolescence, it might be best to have the child return to school, when offered. This IS the new normal, and for those who are less affected with anxiety or communication delay, the experience is important. For those patients who are significantly delayed in language or behaviors, this is the time when some parents have observed, that, maybe ‘regular’ school isn’t the best placement.
Teens who are ‘on the spectrum’ have usually already displayed their level of ability to weather stormy environments. They have, after all, been doing it all of their lives! Parents can usually take their cues from the child’s strengths and weaknesses. The most affected or immature are usually in a special needs environment. However, this age group appears to be the least sensitive to dire medical outcomes, so returning to school is important. That could lead to key decisions about interaction with high risk family members. It is crucial for those kids who have been drowning in a digital ocean to head back toward reality. As soon as possible, scheduling daily decreases in screen time to a reasonable level might be prudent.
IMPORTANT SIGNS & SYMPTOMS
Speech apraxia – Continuation of therapies is paramount. TheAutismDoctor.com has many blog posts about the need to aggressively attack this issue in order to achieve life-long improvements. If the child has any inclination toward speaking at all, run- do not walk- to continue that treatment protocol, and reinforce it with the correct professional speech and language strategies. Academic pursuits are certain to be more effective when communication is optimized.
Aggressive behaviors – Does the child exhibit poorer self-control in or out of school? There are those who, “only hit the ones they love,” and other affected individuals who react very negatively to transitioning to non-preferred behaviors – which is what school is for them. For those children who require substantial or very substantial support, perhaps this is the time when parents can really assess what is the actual best place – school notwithstanding (which it isn’t during lockdown).
Focus, Attention – Does distractibility lead to loss of concentration, inability to focus lead to too much fidgeting, or does fidgeting and over-activity lead to the loss of attention? Although teasing out the primary difficulty may be nearly impossible, finding such a nuance about your child’s inability to learn – even though you know that they are smart – could yield the difference between effective therapy (including biomedical intervention, ‘neurofeedback’, etc.) or potent medications with possible harmful side effects. Does the child learn better in or out of school, and is it worthwhile to administer medications so that they can be more successful in an academic environment, especially when there may be many stops and starts to the coming semesters.
Hyperactivity – Some children seem to be able to sit surprisingly still at school, but have major problems when a digital device, food, or siblings are in the vicinity. Most overly active children, however, do enjoy the ability to learn when they have “gotten the willies out’, been given a snack, or allowed time to do a preferred activity for a bit. Can they learn better at home? Do you have the resources to keep up that home school? What will happen when school does get back in session? Many youngsters on ADHD medications have been on a ‘holiday’ since Quarantine. That begs the question, “How important are pharmaceuticals simply to get Mini-Me into a schoolroom?” Usually, in ‘real’ life… all things being equal… the answer (depending on the child’s age) is, “During school, Yes!” However, the present pandemic may postpone that prescription.
Social inadequacies – It appears that behaviors range from none- to too much, too loud, too often – to extremely rude, frequently requiring discipline, and inability to get along. Often, the children have processing issues that are manifest as downstream sensory, oppositional, or attention ‘disorders’, that further their isolation and anxiety. Likewise, the decrease in anxiety that many of our parents have noted has caused a re-evaluation of their previous educational situation. Decisions about disposition to school, etc.? in this domain are mostly age-related, and more important as language emerges and less so, as coping skills require some distance and become more hard-wired.
RESOURCES
Time – As venues open and close, families’ ability to assess the ‘when, how, and where’ of their children’s disposition to school is already in tremendous flux. The virus is winning at this time, so the ‘matrix’ of decision-making starts and ends with infection rates.
Personnel – There are families with one child and 2 or 3 therapists, and others with five children but no professional support. As this pandemic forges its way across the world’s population, planning for more at-home strategies may become even more critical, especially for this next year. Lining up teachers and therapists – real and virtual – will provide a valuable cushion, should more chaos ensue.
Money – Insurance, supplements, medications, even food and shelter have become more uncertain. As parents try to assess the best course for their developmentally-challenged child, there is no doubt that the basic necessities are just that. School attendance may confer some increased risk, but is preferable to remaining in the house without any significant preparation.
Family situation – It is not unusual for families today to have at least one household member who may suffer from some auto-immune or other high-risk condition that could result in significant illness or even death, should COVID-19 strike. Such situations might be ameliorated by more frequent and reliable testing, for sure. In the meantime, the child(ren) and at-risk family member(s) obviously must take extraordinary measures, should return to school be the most likely choice.
Conclusions
The only way that we will navigate out of this present mess is to listen to the science. It changes. It’s not perfect. It’s unpredictable. It’s mysterious. We don’t understand the virus and so we cannot control it. And the only thing that we do know is that masks help (and we aren’t even sure why!). Hand-washing should be a no-brainer. This is not political.
Our experience at The Child Development Center of America has been that approximately 1/3 of patients (all ages) are going to go (or already have gone) back to school. One third are definitely not going back. The other third are waiting for local medical and government leadership to provide instruction, often based on parent surveys, on what to expect this fall and winter.
In the absence of any abundance of useful guidance, following this process may assist in the infinite love and wisdom of our warrior-parents.
Also see:
COVID-19 Planning Considerations: Guidance for School Re-entry
Critical Updates on COVID-19 / Clinical Guidance / COVID-19 Planning Considerations: Guidance for School Re-entry
What Will Schools Do When a Teacher Gets Covid-19?
Cases are inevitable. Schools need to plan now.




