There isn’t one presentation of autism. Plus, there are multiple causes of the childhood developmental challenge that is characterized by certain behaviors and communication delays known as Autism Spectrum Disorder. Symptoms are often linked to underlying conditions; such as genetic, inflammatory, auto-immune, toxic, and / or metabolic alterations either alone or actors in a vicious cycle.
As a result of nutritional or metabolic changes, or as a possible primary condition, a diminished level of brain fat, as reflected by low serum cholesterol, is identifiable. The consequences could well appear as a lack of attention, crossed connections, unresponsiveness, and delayed maturation. In this manner, it is a measurable and treatable medical condition.
Brain fat?
Cholesterol is mostly known for its negative role in arteriosclerosis, creating plaque that can block flow to organs, such as the heart or brain. However, specific fats play a major part in proper Central Nervous System (CNS) operations. This fatty substance helps provide Insulation, conduction, and the framework for correct functioning and fiber regeneration from loss or damage.
Nerve impulses start at one end (dendrite) of a fiber (axon) and end at a point (terminal) where electrical signals pass on via chemical transmission (neurotransmitters) to the next branch. That ‘wire’ is encased in an enveloping sheath which is produced by specialized cells (Schwann cells), and is made of a predominantly cholesterol-containing substance (myelin). It is easy to imagine that the developing brain must require large amount of such a substrate. 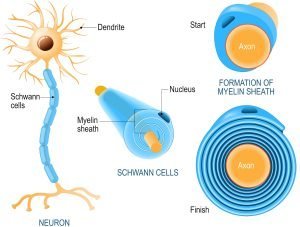 This situation is quite similar to an electrical circuit, as can be seen in this engineering diagram.
This situation is quite similar to an electrical circuit, as can be seen in this engineering diagram.
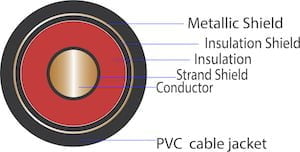 Now, picture bare wires and poor insulation – leading to incorrect, crossed or no circuits at all!
Now, picture bare wires and poor insulation – leading to incorrect, crossed or no circuits at all! Clinical Experience
Clinical Experience
Regarding this condition and intervention, here are some points that the staff at The Child Development Center has learned along the way:
1. There is some kind of relationship between the ~85% of our patients who present with a low Vitamin D3* level and the 5-10% who demonstrate very low cholesterol levels (diagram). Maintaining adequate levels of both is an important step in normalizing either.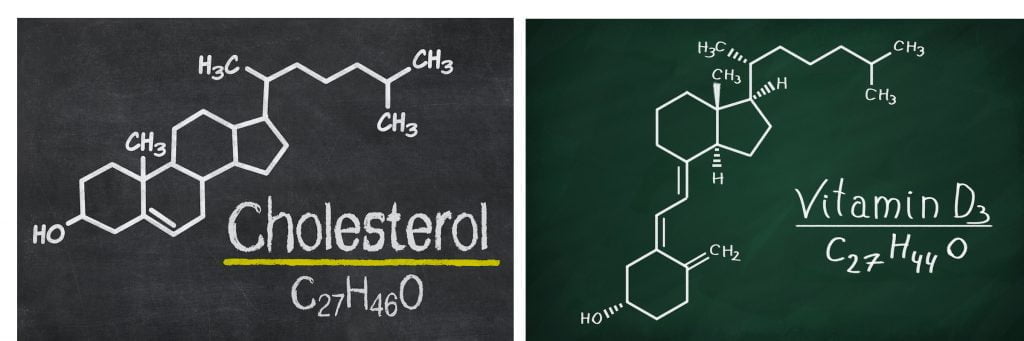 2. Sonic cholesterol, a proprietary ‘medical food’, is the preferred treatment protocol at our Center. We usually start with 2 or more capsules, and titrate depending on the initial, then subsequent, serum levels. (A ‘Google’ search for products that raise serum cholesterol yields the same result.)
2. Sonic cholesterol, a proprietary ‘medical food’, is the preferred treatment protocol at our Center. We usually start with 2 or more capsules, and titrate depending on the initial, then subsequent, serum levels. (A ‘Google’ search for products that raise serum cholesterol yields the same result.)
3. The most immediate improvements are visible as evidenced by better eye contact and the patient seeming to be more ‘connected’. Activating protocols, such as methyl B12 injections or Folinic acid, may be more effective once the CNS electricity is flowing correctly.
4. The follow-up total serum cholesterol level is often LOWER than the original! Symptoms have improved by then, and it appears that the intervention successfully assisted in sending the ingested fat to the brain. That usually prompts an increase in dosage. Cholesterol levels are checked 2-3 times per year, thereafter, to assure that the level is correcting but doesn’t become elevated.
5. Conversely, more than 75% of our patients exhibit increased total cholesterol levels. Pediatricians (myself included) do not generally treat elevations in total serum cholesterol, and this finding deserves further research and evaluation.
Short Q & A with Dr. Udell
What level of cholesterol is considered too low?
![]() I am generally concerned about levels that are ~10% lower than the laboratory ‘low normal’. Some labs do not list such a range, so a level that is less than 125 mg/dl, for example, might need to be addressed.
I am generally concerned about levels that are ~10% lower than the laboratory ‘low normal’. Some labs do not list such a range, so a level that is less than 125 mg/dl, for example, might need to be addressed.
Why does my child have a low cholesterol?
![]() There are some medical diseases (SLOS, e.g.) that involve a genetic alteration in cholesterol synthesis. In our experience, we have not determined a consistent causative or associated factor (other than Vitamin D3). Evidence-based scientific information is now emerging.
There are some medical diseases (SLOS, e.g.) that involve a genetic alteration in cholesterol synthesis. In our experience, we have not determined a consistent causative or associated factor (other than Vitamin D3). Evidence-based scientific information is now emerging.
How long will the treatment go on?
![]() Serum levels determine the course. Some patients have corrected within months, some within years, and some continue to experience improvements, but require either continuous or intermittent intervention. The goal is to be within range of normal lab values.
Serum levels determine the course. Some patients have corrected within months, some within years, and some continue to experience improvements, but require either continuous or intermittent intervention. The goal is to be within range of normal lab values.
What about dietary increases with more eggs, bacon, and other high cholesterol-containing foods?
![]() I want to be sure that the patient doesn’t form IgG antibodies to eggs, for example, that may increase an inflammatory load, before suggesting ‘helpful’ foods.
I want to be sure that the patient doesn’t form IgG antibodies to eggs, for example, that may increase an inflammatory load, before suggesting ‘helpful’ foods.
![]() The goal is delivery of the correct fat to the brain, not the coronary arteries. Elevated total cholesterol levels in any patient should be of concern for later years.
The goal is delivery of the correct fat to the brain, not the coronary arteries. Elevated total cholesterol levels in any patient should be of concern for later years.
![]() Experience has shown that diet alone is not effective.
Experience has shown that diet alone is not effective.
What if other items that appear in a lipid profile, such as triglycerides, HDL, LDL are out of range?
![]() That is another factor that deserves further investigation and knowledge. Our position on the whole issue may be simplistic, but it is safe, relatively inexpensive, and quite useful.
That is another factor that deserves further investigation and knowledge. Our position on the whole issue may be simplistic, but it is safe, relatively inexpensive, and quite useful.
Have there been any negative effects from the medical food?
![]() Not as long as we continue to monitor growth, development, and appropriate laboratory values.
Not as long as we continue to monitor growth, development, and appropriate laboratory values.
Conclusion:
Notwithstanding all of this scientific jargon, here is a simple take-home message:
If you are the least bit concerned about your child’s development, ask your pediatrician to perform a basic childhood developmental scale and the following laboratory tests:
Complete Blood Count (CBC)
Comprehensive metabolic panel (CMP)
Lipid Profile
Ferritin level
Thyroid screen (TSH)
Vitamin D3 level
You – and your doctor – may be surprised at the results! Correcting anemia, discovering a thyroid issue, advancing functioning with safe, easy to obtain ingredients may provide a wake-up call for further useful medical investigation and successful interventions.




Dr. Udell,
I am a psychotherapist in private practice. I have worked with other adults on the spectrum, but have a 28-year old young man I am working with who I believe is on the spectrum due to psychosocial history I’ve taken and his score on the Autism Quotient scale (34). He has issues with reflux, IBS, and has a hiatal hernia in addition to high anxiety. We are working with some coping tools, but need more resources for information for adults with Autism and the above health issues. I would appreciate any studies, resources you may have. Many thanks, Donna Henn, M.S., LPC
Adults who are diagnosed with ASD is an entirely OTHER specialty that needs to be developed. Unfortunately, the present treatments involve potent medications to control behaviors (with limited success). Basically, the original diagnosis of autism is lost to schizophrenia, bipolar disorder, severe anxiety or depression. With the ever-increasing incidence of new cases of affected children, hopefully a new paradigm will engender a more modern approach.
My practice is basically treading water trying to prevent those more-affected adults from going in the wrong direction. It’s a struggle as the legal, medical, and hospital systems are unaware of their proper involvement in this burgeoning epidemic.
Is it normal for a non verbal 4 year old childs
Calprotectin (alpha) be 863 ug/g
They say he has infection of the intestines
Elevated levels should be evaluated.