If the holy grail of HBOT therapies is to promote new neural connections, then the gold standard of objective evidence could be this technology. Single photon emission computed tomography creates images of the brain which combine multiple 2-D views left by a special chemical (which is injected into a patient’s arm). Multiple pictures are taken from multiple angles and a computer reconstructs the image into the 3D views. Images provide detail down to 1/2 inch – not as good a s some technologies but a lot less expensive (~$1,000 plus*).
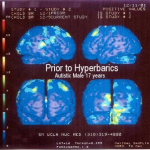 By combining this smart camera with the right type of tracer chemical, the radiologist can interpret brain blood flow. As noted in the previous post, such information represents the most tangible evidence that a patient has/could/would/may/should improve on continued HBOT therapy.
By combining this smart camera with the right type of tracer chemical, the radiologist can interpret brain blood flow. As noted in the previous post, such information represents the most tangible evidence that a patient has/could/would/may/should improve on continued HBOT therapy.
In the best of all worlds, a SPECT scan would be performed before starting HBOT, then after twenty sessions or so. Even in the absence of clinical improvement, that knowledge may make a parent want to continue 40, 60, or more treatments..
Conversely, lack of change in blood flow may influence the decision about continuation of HBOT. Any symptomatic improvements could have been due to improved G-I health or sensory conditioning, rather than an HBOT – Brain specific relationship.
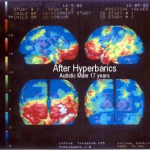
To choose such a protocol would involve twice the anesthesia, more exposure to radiation (however small), increased financial burden, extra time and lots of stress. However, SPECT scanning is a very interesting technology that may help a family better understand their child’s condition and reaction to the controversial and resource-intensive treatment of HBOT.
The lingering question remains, “Does increased oxygen delivery indicate, or lead to, or in some way promote (and in no way worsen) infantile autism?” This technology may be the best information that we have for now, concerning the usefulness of this expensive and time-consuming technology of HBOT.
*The costs will go up depending on the chemical that is injected, whether/type of anesthesia, interpretation by a trained radiologist and any other additions that they can think of.
One more post to go! (about this topic, for now)




heya, excellent site, and a decent understand! 1 for my favorites.
good and useful information,i will come back later.
Thanks for the info. This was very interesting.=)
band it tool
I had a good time here but will return to google now.
Your page is looks mercy, your graphics are sweet, and what’s more, you use reference that are relevant to what you are saying!2$
Hello. My name is Kimberly Livings, pleased to meet you.
I was reading into this subject when I came across your blogpost “SPECT Scans and Autism Spectrum Disorder theautismdoctor.com”. At this time I have a blog myself (https://www.theautismdoctor.com//www.buyexhaustmuffler.com/ducati). … It might be a little offtopic but still, take a look the blog 🙂
Thanks,
Kimberly Livings of https://www.theautismdoctor.com//www.buyexhaustmuffler.com/ducati
Interesting layout on your blog. I really enjoyed reading it,I will be back to read more in the future.
Hi there! I could have sworn I’ve been to this site before but after reading through some of the post I realized it’s new to me. Anyhow, I’m definitely glad I found it and I’ll be book-marking and checking back often!
fascinating webpage about SPECT Scans and Autism Spectrum Disorder theautismdoctor.com. I read it three times!.
Now i know, thanks for the info, I value your opinion alot more.:)
My friend and I want to let you know that we loved visiting on this page, I was just interested to know if you barter featured posts? I am always attempting to find bloggers to make deals with but it’s merely a point of view I would call for.
Umm… if I can get a link, that will be fine for now.
loved this thanks
Your place is valueble for me. Thanks!…
Dam this Blog is AWESOME. If you wrote this any better i would think you were a super human. lol nice.:)
Its always cool to arrive along a site like yours that has this type of topics to read about. Thoroughly enjoyed and will definitely be returning often
With all the blooming snow I have had as of late I am stuck inside , fortunately there is the internet, cheers for leaving me something to do
tnx buddy
about the most recent posts are fantastic quality bootcamp guess I’ll add you into my daily bloglist,would you mind writing your weblog with even more data.2$4
This post has been extremely helpful to me. There have been many posts on this subject before, but yours nailed it. I will share this since I know a lot of others who would love it too.
This site is a great way to reach out to others. Congratulations on a task well accomplished. I am expecting your next entry.
Having just been looking for useful blog posts for the research project I’ve been working on when I happened to find yours. Thanks for this informative material! — Sergio Arterbury
Hi I like this post and it is so fabulous and I am definetly going to save it. One thing to say the Indepth analysis you have done is trully remarkable.No one goes that extra mile these days? Bravo!! Just another suggestion you shouldinstall a Translator Application for your Worldwide Audience …
Working on the tech stuff. Thanks
This is absolutely a great post. My only issue is I am having an issue with your RSS feed . For some reason I am unable to subscribe to it. Is there anybody have an similar RSS problem? If anybody else is having a similar issue please contact me Hurter1661@gmail.com.
Yeah, lotso comments re:rss. New web person this week.
My brother suggested I might like this blog. He was entirely right.
This post actually made my day. You can not imagine simply how much time I had spent
for this info! Thanks!
It is truly a great and helpful piece of information. I am glad that you just shared this useful information with us.
Please keep us up to date like this. Thanks for sharing.